Necrotising fasciitis as a complication of varicella in children
Varicella is a common and simple infectious disease in children, but necrotising fasciitis sometimes can be a complication, presenting as a rapidly progressive soft tissue infection that can be lethal. In this article, we present 4 children that had been diagnosed…
AUTHORS: Santino Figueroa Ángel * M.D , Venecia Romero Flores ** M.D
* Surgeon corresponding to the department of Plastic and Reconstructive Surgery at Hospital Infantil of Mexico Federico Gómez and Hospital Regional Licenciado Adolfo López Mateos. Mexico city, MÉXICO. Plastic Surgeon and General Surgeon
** Surgery resident at Hospital Regional Licenciado Adolfo López Mateos. Mexico city.
ABSTRACT
Varicella is a common and simple infectious disease in children, but necrotising fasciitis sometimes can be a complication, presenting as a rapidly progressive soft tissue infection that can be lethal. In this article, we present 4 children that had been diagnosed with varicella and complicated with necrotising fasciitis. We describe their clinical characteristic as their age, sex, the presentation of the disease, location of the infection, history of NSAID consume, symptoms at time of admission, surgical treatments and complications.
Necrotising fasciitis affects children differently than it does to adults. It is usually present in healthy children with a relatively unremarkable medical history. Early diagnosis and prompt medical and surgical treatment is essential to improve recovery and outcome.
Keywords: Necrotising fasciitis; Varicella zoster,
NECROTISING FASCIITIS AS A COMPLICATION OF VARICELLA IN CHILDREN
Although varicella is a minor, self-limited, superficial infection in children; the disease can be associated with a variety of serious complications (1). Skin and soft tissue infections are the most frequent complications of chicken pox in children, and it is usually caused by Staphylococcus aureus or Streptococcus pyogenes (2,3). Bacterial infection occurs by direct invasion, usually after trauma (4).
The earliest signs of necrotising fasciitis (NF) are oedema and erythema. As the infection worsens, bullaes with clear fluid transform into a haemorrhagic fluid. The infection progresses rapidly, spreading along fascial planes beyond the margins of erithema, with the subsequent proliferation of the microbial pathogen in the superficial fascia, releasing enzymes, toxins and endogenous cytokines that produce liquefactive necrosis (5- 9).
MATERIAL AND METHODS:
We present 4 cases of necrotising fasciitis secondary to a varicella infection in children, in whom diagnosis was made upon clinical characteristics, in a period comprised from 2008-2010, treated by the Plastic and Reconstructive Surgery Departments at the “Hospital Infantil de México Federico Gómez” and “Hospital Regional Licenciado Adolfo López Mateos”, in Mexico City, Mexico.
RESULTS:
This study includes 4 cases, (3 girls and 1 boy), ages ranging from 2 to 12 years, without a relevant medical history. The time of duration from the appearance of vesicles to clinical necrotising fasciitis ranged from 4 to 7 days. The site of infection was different for each patient.
Every patient at time of admission, showed signs of systemic inflammatory response and had clinical signs of necrotising fasciitis, ranging from bullaes, skin discoloration, and skin and soft tissue necrosis. Only 2 patients showed foul smelling purulent discharge. An elevated leukocyte count was present in all. Only the patients of clinical case number 1 and 2, showed alterations of renal function as a result of elevation of urea and creatinine, and were hypotensive at time of admission, but responded rapidly to IV fluids and resuscitation. The patient of clinical case number 1 also showed at admission, hyperglycemia, thrombocytosis and an elevation of Total bilirubine to 1.4 mg/dL and direct bilirubine to 1.25 mg/dL.
The first debridement was promptly done in less than 12 hours in most patients, and the maximum of subsequent debridement procedures were 4. Local wound care was given every day and I.V broad spectrum antibiotics were received, and only one patient received fungical antibiotic because of a hemocultive positive for candida parapsilosis. Only 3 of the cultures taken, were positive: 2 cultures showed Streptococcus pyogenes, and one showed Staphylococcus aureus.
Figure Legends:
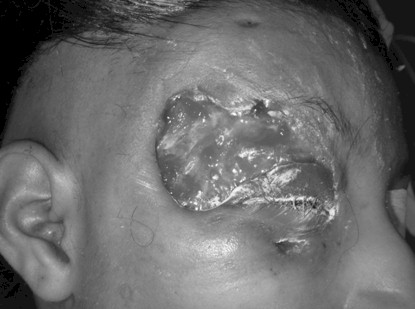
Figure 1: Patient corresponding to the clinical case number 1, on the operating room, before the taking and placement of the full thickness skin graft as aesthetic units, from the right groin. (21st day)
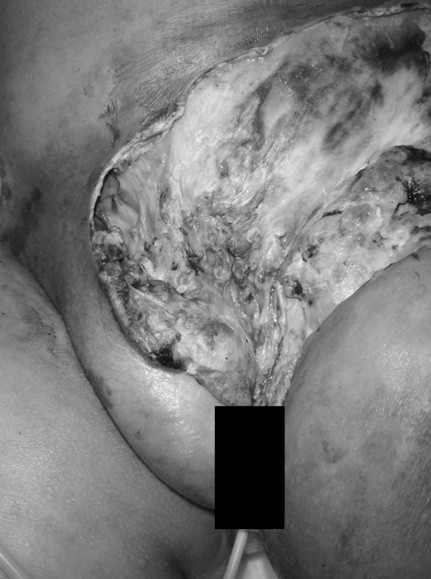
Figure 2: Patient corresponding to the clinical case number 2, on her first evaluation, at time of admission. Note the areas of necrosis and exudate.
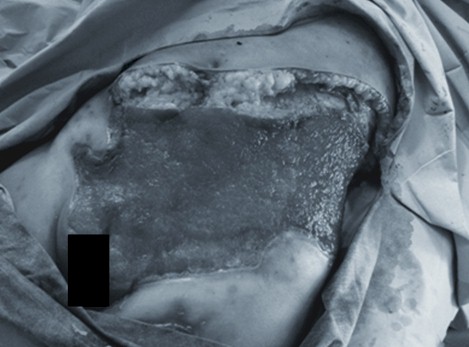
Figure 3: Patient of clinical case number 2, 3 weeks later, showing how the lesion extended further after the first evaluation, now presenting a healthy granulation tissue, ready to be grafted.
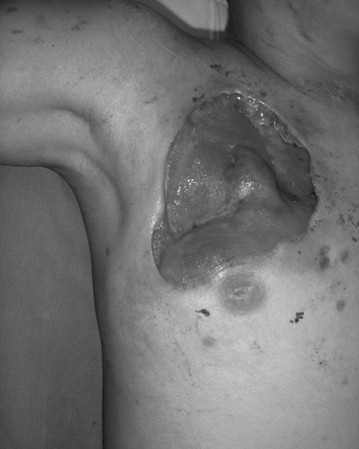
Figure 4: Patient of clinical case number 3, showing her right upper trunk lesion at the third week of admission, ready to be grafted.
Figure 5: Patient of clinical case number 4, at the third week of admission, now that the infection has faded. Note the multiple scars as sequels.
The final surgical interventions were a full thickness graft in one patient, a meshed split-thickness skin graft in one patient, a split-thickness skin graft in one patient, and advancement of superior and inferior flaps in one patient. Only the patient of the clinical case number 1 required two surgical interventions; the second intervention needed to remodel a superior eyelid retraction.
TABLE 1: CLINICAL FEATURES OF THE 4 PATIENTS
Features PATIENT 1:
Age (years): 12
Sex: Female
Comorbidities or Immuno-compromise: No
NSAID history: Paracetamol
Presentation: 5 days after the onset of varicella, the girl presented right hemifacial oedema plus right sided periorbital pain and erythema , which progressed to a periorbital ulceration in 48 hours.
At admission: Cellulites, partial skin and soft tissue necrosis, crepitus, and foul purulent discharge.
Affected area: Right periorbital and temporal region.
Symptoms and systemic signs at admission: Fever, malaise, hypotension, tachycardia, tachypnea.
First debridement after admission: < 8 hours
Antibiotics used: Vancomycin, Meropenem, Metronidazole, Fluconazole**
Bacteria isolated from culture: None
Reconstruction surgery: Full thickness skin graft. (Two interventions)
Complications of the infection: Hemocultives positive with candida parapsilosis & Scars.
Hospital: Hospital Regional Licenciado Adolfo López Mateos
Features PATIENT 2:
Age (years): 7
Sex: Female
Comorbidities or Immuno-compromise: No
NSAID history: Paracetamol, Ibuprofen
Presentation: At the 4th day of the diagnosis of varicella, small ulcerations and a zone of erythema, rapidly progressed to become a large necrotic area within days.
At admission: Necrosis of skin, soft tissue and aponeurosis, plus crepitus and foul purulent, gray discharge.
Affected area: Low abdominal Wall and left inguinal region.
Symptoms and systemic signs at admission: Fever, irritability, malaise, hypotension, tachycardia, tachypnea.
First debridement after admission: < 12 hours
Antibiotics used: Penicillin, Gentamicin, Clindamycin
Bacteria isolated from culture: Streptococcus pyogenes and E. colli
Reconstruction surgery: Mesh, split-thickness skin graft
Complications of the infection: Hypertrophic Scars.
Hospital: Hospital Infantil de México Federico Gómez.
Features PATIENT 3:
Age (years): 8
Sex: Female
Comorbidities or Immuno-compromise: No
NSAID history: Methamizol
Presentation: 7 days after the appearance of vesicles, rapid confluent ulcers and skin discolorations appeared in the trunk, progressing to a cruent area.
At admission: Necrosis of skin, soft tissue and mayor pectoral aponeurosis, without discharge.
Affected area: Right pectoral area.
Symptoms and systemic signs at admission: Malaise, anorexia and Pain.
First debridement after admission: < 16 hours
Antibiotics used: Penicillin, Clindamycin
Bacteria isolated from culture: Streptococcus pyogenes
Reconstruction surgery: Split-thickness skin graft.
Complications of the infection: Minimal scars.
Hospital: Hospital Infantil de México Federico Gómez.
Features PATIENT 4:
Age (years): 2
Sex: Male
Comorbidities or Immuno-compromise: No
NSAID history: Methamizol
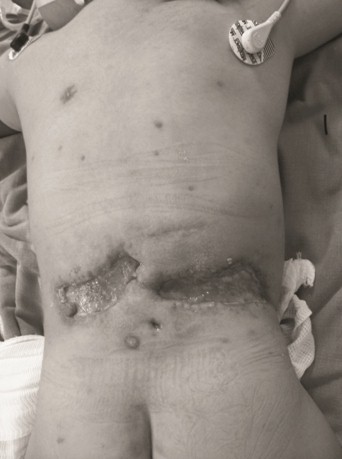
Presentation: At the 4th day after the onset of varicella, the boy presented fever, malaise, erythema, oedema of lower back, plus bullaes formation transforming into hemorrhagic.
At admission: Haemorrhagic Bullaes, skin discoloration and soft tissue necrosis, plus serohematic discharge.
Affected area: Lower back.
Symptoms and systemic signs at admission: Fever, malaise, irritability.
First debridement after admission: < 12 hours
Antibiotics used: Penicillin, Clindamycin
Bacteria isolated from culture: Staphylococcus aureus
Reconstruction surgery: Advancement flaps.
Complications of the infection: Minimal scars.
Hospital: Hospital Infantil de México Federico Gómez.
DISCUSSION:
Necrotising fasciitis is commonly present in adults with comorbidities, but the difference with children is that it can occur in previously healthy kids, with a history of trauma to the skin. Acute cases show a progression of signs and symptoms in days (10), and all of our patients were considered acute cases. Early recognition, antibiotic impregnation and emergency surgical exploration and debridement are essential to avoid life threatening complications (11). Some authors suggest as a first line antibiotic, the use of high-dose penicillin G or cephalosporin, plus clindamycin or metronidazole, with or without an aminoglycoside (12,13).
Necrotising fasciitis can be seen everywhere in the body but it is more common in the abdominal wall, extremities and Perineum (14). Periorbital involvement is rare (15), and Luksich et al. recommends a conservative approach if the infection shows no sign of extension into the orbit (16). Some authors recommend that all patients without signs of sepsis can be safely managed with medical treatment to allow the necrotic areas to auto-demarcate, and then, the necrotic tissue should be debridement as needed (17).
The diagnosis of necrotising fasciitis is clinical. Magnetic Resonance Imaging is useful to differentiate between necrotic soft tissue infection and edematous tissue (18), but treatment should not be delayed just to obtain a study.
In a 13 months surveillance study throughout the UK and Ireland, 12 of 112 children had varicella complicated with a soft tissue infection, being necrotising fasciitis present in 7. Of the cultures taken, they could only confirm a specified microbiological agent in 6 patients, being the most frequent a Group A Streptococcus (19). In our study, only 3 patients had positive cultures, being the most common isolated bacteria, a Group A Streptococcus.
There are 3 risk factors that predict mortality in patients with necrotising fasciitis: advanced age, immunocompromise, and streptococcal toxic shock syndrome (20). None of our patients had those risk factors, and everyone had a prompt surgical and medical treatment, and we didn’t have any lethal complication.
Some authors have suggested a possible association between the use of non-steroidal anti-inflammatory drugs and an increased risk of varicella-associated necrotizing fasciitis, although this association remains controversial (21). In Mexico the use of paracetamol and methamizol in children is frequent and it was present in the medical history of all of our cases, but we cannot certainly affirm the association of its use and the presence of necrotising fasciitis.
CONCLUSIONS
It is essential to make an early diagnose of necrotising fasciitis and begin with a prompt treatment with IV antibiotics, IV fluids, and surgical debridement. Sometimes, many debridements are going to necessary, especially if done early, as necrosis may progress. Some patients presenting with septic shock should be aggressively treated to avoid lethal complications. If the patient is stable and non septic, the first debridement can be delay to allow necrotic tissue to demarcate. Reconstruction techniques are plenty and vary depending on the affected area, diameter, and clinical status. Every reconstruction technique must be individualized in each patient.
ACKNOWLEDGEMENT: NONE
Conflict of interest: None.
Funding: None.
REFERENCES
(1). Gnann JW Jr. Varicella-zoster virus: atypical presentations and unusual complications. J Infect Dis. 2002 Oct 15;186 Suppl 1:S91-8.
(2). Snel BJ, Visconti G, Grabietz PD, Werker PM. Necrosis of nose skin after varicella zoster infection: a case report. J Plast Reconstr Aesthet Surg. 2010 May;63(5):e445-7.
(3) Peterson CL, Mascola L, Chao SM, et al. Children hospitalized for varicella: a pre-vaccine review. J Pediatr 1996; 129:529-36
(4). Dryden MS. Skin and soft tissue infection: microbiology and epidemiology. Int J Antimicrob Agents. 2009 Jul; 34 Suppl 1:S2-7.
(5). Green RJ, Dafoe DC, Raffin TA. Necrotizing fasciitis. Chest 1996; 110: 219–29.
(6). El-Khani U et al. Multifocal necrotising fasciitis: An overlooked entity?. J Plast Reconstr Aesthet Surg. 2011 Sep 24.
(7). Chapnick EK, Abter EI. Necrotizing soft-tissue infection. Inf Dis Clin N Am 1996; 10: 835–55.
(8). Shirley R, Mackey S, Meagher P. Necrotising fasciitis: a sequelae of varicella zoster infection. J Plast Reconstr Aesthet Surg. 2011 Jan;64(1):123-7. Epub 2010 Jun 8.
(9). Moss RL, Musemeche CA, Kosloske AM. Necrotizing fasciitis in children: prompt recognition and aggressive therapy improve survival. J Pediatr Surg. 1996 Aug;31(8):1142-6.
(10). Whallett EJ, Stevenson JH, Wilmshurst AD. Necrotising fasciitis of the extremity. J Plast Reconstr Aesthet Surg. 2010 May;63(5):e469-73. Epub 200
(11). McHenry CR, Piotrowski JJ, Petrinic D, Malangoni MA. Determinants of mortality for necrotizing soft-tissue infections. Ann Surg 1995; 221: 558–63.
(12). Vinh DC, Embil JM. Rapidly progressive soft tissue infections. Lancet Infect Dis. 2005 Aug;5(8):501-13.
(13). Moss RL, Musemeche CA, Kosloske AM. Necrotizing fasciitis in children: prompt recognition and aggressive therapy improve survival. J Pediatr Surg. 1996 Aug;31(8):1142-6.
(14). El-Khani U et al. Multifocal necrotising fasciitis: An overlooked entity?. J Plast Reconstr Aesthet Surg. 2011 Sep 24.
(15). Snel BJ, Visconti G, Grabietz PD, Werker PM. Necrosis of nose skin after varicella zoster infection: a case report. J Plast Reconstr Aesthet Surg. 2010 May;63(5):e445-7.
(16). Luksich JA, Holds JB, Hartstein ME. Conservative management of necrotizing fasciitis of the eyelids. Ophthalmology 2002; 109:2118e22.
(17). Fung V, Rajapakse Y, Longhi P. Periorbital necrotising fasciitis following cutaneous herpes zoster. J Plast Reconstr Aesthet Surg. 2012 Jan;65(1):106-9. Epub 2011 Jul 23.
(18). El-Khani U et al. Multifocal necrotising fasciitis: An overlooked entity?. J Plast Reconstr Aesthet Surg. 2011 Sep 24.
(19). Cameron JC, Allan G, Johnston F, Finn A, Heath PT, Booy R. Severe complications of chickenpox in hospitalised children in the UK and Ireland. Arch Dis Child. 2007 Dec;92(12):1062-6. Epub 2007 Nov 8.
(20). Golger A, Ching S, Goldsmith CH, Pennie RA, Bain JR. Mortality in patients with necrotizing fasciitis. Plast Reconstr Surg. 2007 May;119(6):1803-7.
(21). Zerr DM, Alexander ER, Duchin JS, Koutsky LA, Rubens CE. A case-control study of necrotizing fasciitis during primary varicella. Pediatrics 1999;103:7